Infant Data
Results
INDICATIONS
- viral Management in the Newborn

FDA APPROVED INDICATION
Treatment of HIV-1 infection, in combination with other antiretroviral agents, in children starting at birth.
PRECAUTIONS
- Hepatic:
- Lactic acidosis and severe hepatomegaly with steatosis, including fatalities, have been reported; suspend treatment if lactic acidosis or hepatotoxicity (including hepatomegaly and steatosis) are suspected, even without marked elevations in transaminases.
- immunologic:
- Autoimmune disorders, including Graves disease, polymyositis, and Guillain- Barré syndrome, have been reported in the setting of immune reconstitution; may occur many months after initiation of therapy
- Immune reconstitution syndrome has been reported; inflammatory response to opportunistic infections (eg, Mycobacterium avium, cytomegalovirus, Pneumocystis jirovecii pneumonia, TB) may occur during initial phase of antiretroviral therapy.
- Renal:
- Dose adjustment recommended in patients with CrCl of less than 50 mL/min or receiving hemodialysis treatment; monitoring recommended.
ADVERSE EFFECTS
In a 96-week, phase 2, open-label, non-randomized, multicenter study of HIV-infected pediatric patients 3 months to 17 years of age (n=116), skin discoloration, presenting as small, asymptomatic maculae on the palms or soles, occurred in 13% (annual incidence rate) of patients. All cases were mild (grade 1) and self-limiting with one exception (moderate, grade 2). Other common adverse events (all reported as annual incidence rates) were the following: infection (26%), increased cough (17%), otitis media (13%), rhinitis (13%), vomiting (12%), rash (11%), diarrhea (10%), pneumonia (8%), and gastroenteritis (8%). Grade 3 or 4 adverse events considered to be probably or possibly related to emtricitabine included leukopenia, anemia, gastroenteritis, and pancreatitis, all occurring at a frequency of less than 1% (annual incidence rate).
BLACK BOX WARNING
Severe acute exacerbations of hepatitis B (HBV) have been reported in patients who are coinfected with HIV-1 and HBV and have discontinued emtricitabine. Hepatic function should be monitored closely with both clinical and laboratory follow-up for at least several months in patients who are coinfected with HIV-1 and HBV and discontinue emtricitabine. If appropriate, initiation of anti-hepatitis B therapy may be warranted.
ADMINISTRATION
May be administered with or without feedings.
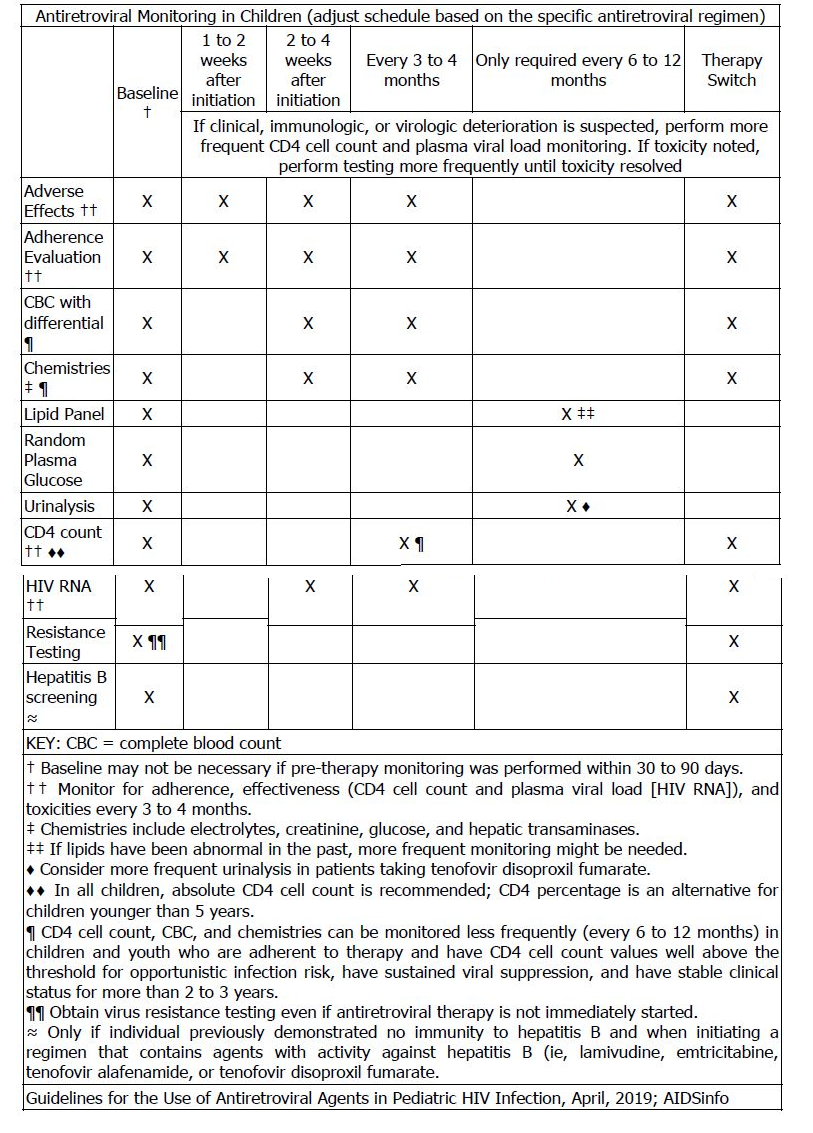
MONITORING